Closure of the left atrial appendage (LAAC)
With this patient information, we would like to welcome you to the Heart Clinic at Mølholm Private Hospital and provide you with information about the treatment.
Our team is dedicated to ensuring that you feel both safe and well-cared for throughout your stay. We aim to provide the highest standard of medical care while fostering a compassionate and supportive environment.
Background for the treatment
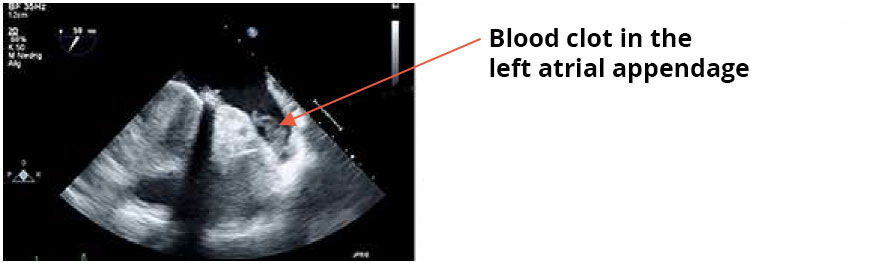
People with atrial fibrillation/flutter have an increased risk of blood clots in the brain. 25% of all strokes are caused by blood clots that form in the heart during atrial fibrillation but then break off and travel to the brain via the bloodstream. Most of these blood clots form in a small "appendage" of the left atrium - the left atrial appendage.
Normally, blood clots are prevented in people with atrial fibrillation using "blood-thinning" medication (Dabigatran, Apixaban, Rivaroxaban, Edoxaban or Warfarin). However, some people are unable to tolerate the medication or have experienced severe bleeding complications. In these cases, the left atrial appendage can be closed using a small closure device, which is inserted into the heart from the groin. The closure ensures that clots cannot form in the appendage, thereby preventing blood clots. Several studies show that protection against stroke after appendage closure is as good as with blood-thinning medication. However, the risk of bleeding is significantly lower without the blood-thinning medication.
Closure of the left atrial appendage can be considered as an alternative to blood-thinning medication, even if there have been no side effects or bleeding complications.
General information
What to bring
Toiletries, slippers, and comfortable clothing. Please also bring your usual medication.
You are welcome to bring a companion, but it is not necessary. You may carry a weekend bag or cabin suitcase with a change of clothes and toiletries, and you may drive or use public transportation (including flying) on the discharge day.
Medication
You should continue your usual medication up to the hospitalization date. However, do not take your morning dose of blood-thinning medication on the day of admission.
If you are being treated with Warfarin, you should ensure in consultation with your doctor that your INR value is between 2.0 and 2.5.
Diuretic medication should not be taken in the morning on the admission day.
If you have diabetes, please follow this link – click here.
Shaving
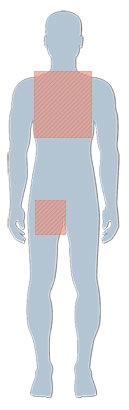
Please remove any hair on your chest and right groin with a disposable razor the day before admission. You should shave the chest and groin corresponding to the shaded area:
Preparation at home (fasting rules)
You must fast from solid food for 6 hours before your appointment time. However, you may drink liquids up to 2 hours before (no dairy products).
You are not allowed to smoke 2 hours before the appointment time.
Visiting hours and phone Contact
You are welcome to bring a companion, but it is not necessary.
Your family members can contact the office during your stay at +45 76 42 74 20. Mobile phones are allowed.
Day of admission
On the day of admission, you will be greeted by a nurse who will help you settle in and provide you with information about your stay. You will be informed of the special precautions that will be taken in connection with the treatment.
Since the treatment time may vary, please expect some waiting time, possibly up to several hours. Regardless of the waiting time, the treatment will be performed the same day.
Your blood pressure and pulse will be measured, and an EKG will be taken. A plastic cannula will be inserted into a vein in your arm, and a single dose of antibiotics will be given to prevent infection.
The treatment itself
The treatment is performed under general anesthesia and is done from the groin.
In the treatment room, there will be several technical devices, including ultrasound equipment, screens, and X-ray equipment. Learn more about the use of X-rays here: X-rays
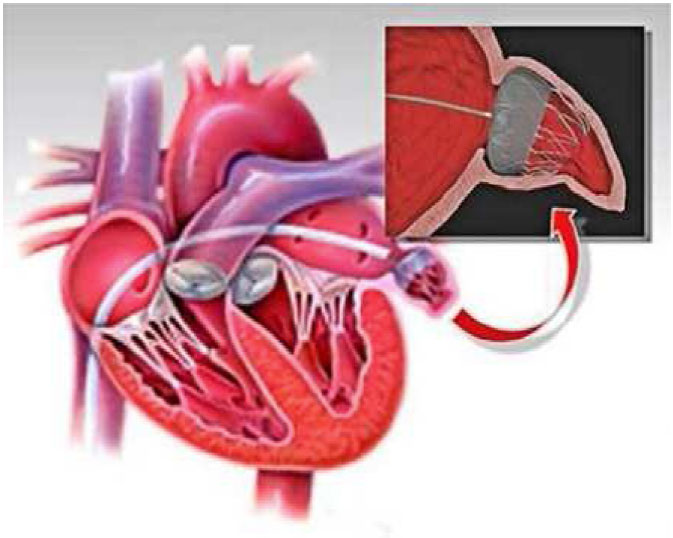
You will be put under full anesthesia, and when you are asleep, local anesthesia will be applied in the groin. Through a vein, catheters will be inserted into the right atrium of the heart and then into the left atrium. The closure device (typically Watchman FLX, Boston Scientific) will be passed through the catheter, and its correct placement will be confirmed using X-ray fluoroscopy with contrast and TEE (an endoscopic examination via the esophagus).
The catheter is then removed, and the puncture site in the groin is closed by compressing the insertion point, with a stitch that will be removed during your hospital stay.
The entire procedure takes about 1½ hours.
Post-treatment
After the procedure, you will be taken to your room on the ward.
You will need to lie flat in bed for 2 hours. It is important that you do not raise your head, upper body, or legs to avoid bleeding. The puncture site will be monitored by a nurse, and your pulse and blood pressure will be measured regularly.
If you feel discomfort, pain, warmth, or swelling in the groin, please inform the nurse.
In rare cases, bleeding may occur from the groin after the procedure, which may require you to stay in bed longer. This bleeding may lead to a hematoma in the groin area, which may cause some pressure over the next few days, especially when walking, but it typically resolves on its own.
You may eat and drink immediately after the treatment.
Medicine
After the procedure, you can skip your blood thinning medication and continue with Aspirin 75 mg for at least 6 months to prevent device related thrombosis (or Clopidogrel if Aspirin is not tolerated). Typically, we recommend continuing with your other medication.
Discharge
You are discharged the morning after the procedure.
Before discharge, the puncture site will be checked, and you will have an ultrasound scan of your heart. You will talk to the treating doctor, and there will be an opportunity to discuss any precautions for the future.
You will receive discharge papers, and we will also send a discharge letter and a description of the treatment to your own doctor and the hospital that referred you for treatment.
You are welcome to drive or use public transportation (including flying) on the discharge day.
You will have a follow-up appointment 3 months after the treatment. During this visit, a follow-up TEE will be performed to ensure that the closure device is still correctly positioned. You will be briefly put to sleep for this examination, and you should fast and bring a family member to drive you home.
You are expected to be discharged from Mølholm after this follow-up.
Complications
Complications from the procedure are rare and may include:
Perioperative complications:
- Blood collection in the groin at the insertion site (risk less than 1%)
- Bleeding into the heart sac (tamponade, risk less than 1%)
- Displacement/embolization of the closure device (risk less than 0.5%)
Postoperative complications:
- Device-related thrombosis (risk less than 0.5%)
- Peridevice leakage (very rare)
If you experience severe shortness of breath, chest pain, dizziness, or fainting, call a medical attention immediately.
It is common to feel tenderness at the puncture site after the procedure.
If you notice signs of infection at the groin site (redness, tenderness, pain, fever), contact us or your own doctor.
In rare cases, there may be bleeding from the groin after discharge. Lie down on the floor and apply firm pressure with your hands to the bleeding site and ask a family member for help. Contact us or another medical facility immediately.
Back home
The day after discharge, you may remove the dressing from the groin if the wound is dry.
During the first week, you should protect your groin by avoiding heavy lifting (2 kg) and long walks. We recommend waiting a total of two weeks before resuming sports.
You can return to your usual work approximately 1 week after discharge. If your work involves heavy physical labor, you should wait 2 weeks.
Hot tubs, spas, and seawater should be avoided for 14 days.
For the first 12 months, you should receive preventive antibiotics (in tablet form as a single dose) for dental visits.
If you are in doubt or have any questions, feel free to contact the Heart Clinic Mølholm by phone at +45 76427420 or email: hjerte@molholm.dk
Speciallæger og behandlere











